How Long Will Medicaid Pay For Hospital Stay . Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Payment policies differ among states and between ffs. Medicaid may impose limits on the length of stay for inpatient hospital services. The use of a provider’s national provider identifier. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. These limits can vary depending on. The exact amount of coverage that medicare provides depends on how long a person. Base payments to hospitals pay for specific services provided to medicaid enrollees.
from www.kff.org
The use of a provider’s national provider identifier. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay for specific services provided to medicaid enrollees. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. Payment policies differ among states and between ffs. These limits can vary depending on. The exact amount of coverage that medicare provides depends on how long a person.
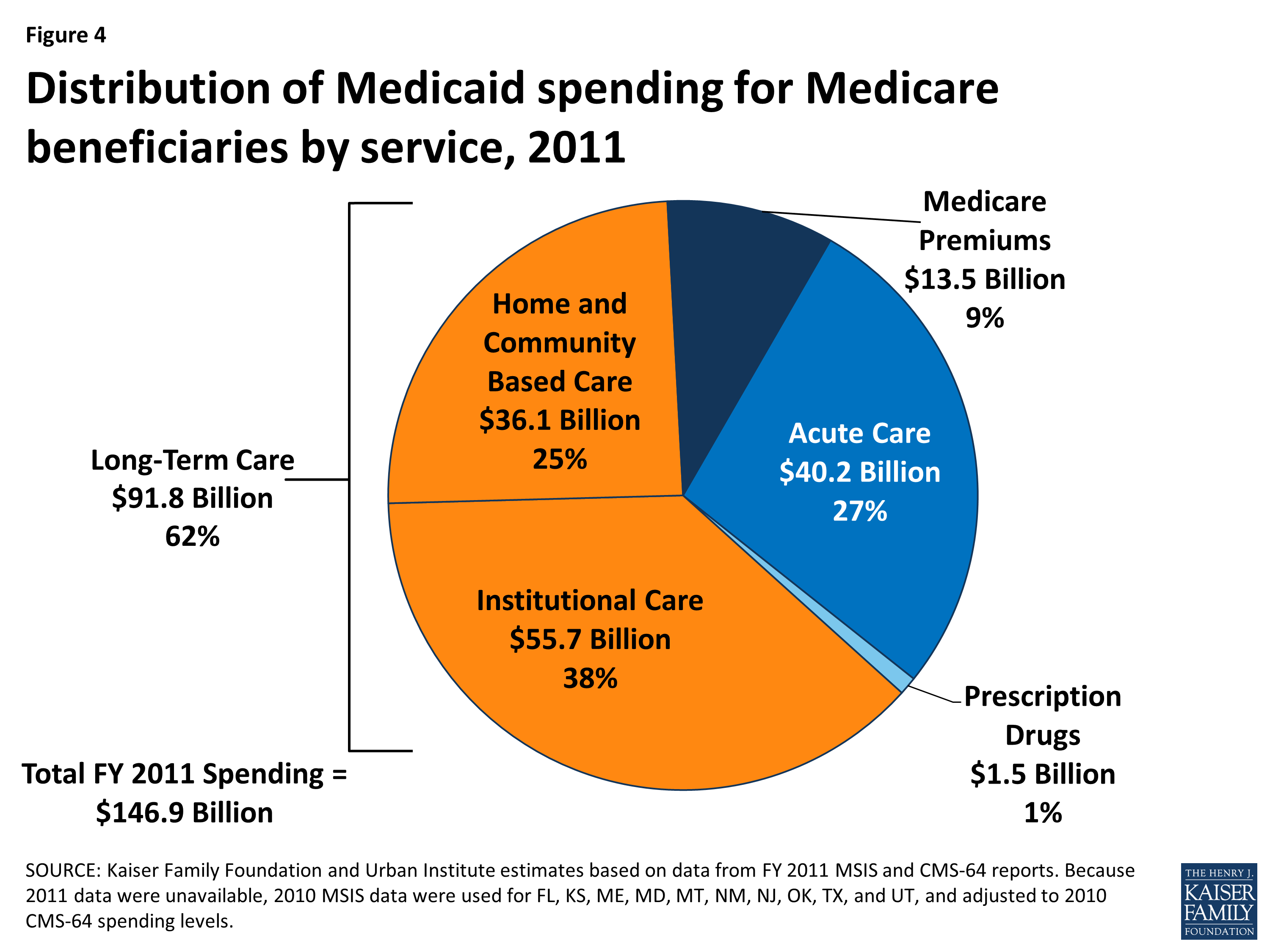
Medicaid’s Role for Medicare Beneficiaries KFF
How Long Will Medicaid Pay For Hospital Stay State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. These limits can vary depending on. Medicaid may impose limits on the length of stay for inpatient hospital services. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. Base payments to hospitals pay for specific services provided to medicaid enrollees. Payment policies differ among states and between ffs. The use of a provider’s national provider identifier. The exact amount of coverage that medicare provides depends on how long a person. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital.
From www.medisupps.com
How Much Does Medicare Pay for Hospital Stay Per Day? How Long Will Medicaid Pay For Hospital Stay The use of a provider’s national provider identifier. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than. How Long Will Medicaid Pay For Hospital Stay.
From www.peoplekeep.com
How much does a hospital stay cost? How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. Medicaid may impose limits on the length of stay for inpatient hospital services. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. The use of a provider’s national provider identifier.. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
Understanding Medicaid Hospital Payments and the Impact of Recent Policy Changes Issue Brief How Long Will Medicaid Pay For Hospital Stay Payment policies differ among states and between ffs. The exact amount of coverage that medicare provides depends on how long a person. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. These limits can vary depending on. Base payments to hospitals pay for specific services provided to medicaid enrollees. In original medicare,. How Long Will Medicaid Pay For Hospital Stay.
From www.medicaretalk.net
Does Medicare Part B Pay For Hospital Stay How Long Will Medicaid Pay For Hospital Stay Base payments to hospitals pay for specific services provided to medicaid enrollees. Payment policies differ among states and between ffs. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. The use of a provider’s national provider identifier.. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
How Much Could Medicare Beneficiaries Pay For a Hospital Stay Related to COVID19? KFF How Long Will Medicaid Pay For Hospital Stay The exact amount of coverage that medicare provides depends on how long a person. Base payments to hospitals pay for specific services provided to medicaid enrollees. The use of a provider’s national provider identifier. These limits can vary depending on. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
A Primer on Medicare How much does Medicare spend, and how does current spending compare to How Long Will Medicaid Pay For Hospital Stay States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. Payment policies differ among states and between ffs. In original medicare, these are additional days that medicare will pay for when you're in a. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
Medicaid’s Role for Medicare Beneficiaries KFF How Long Will Medicaid Pay For Hospital Stay The exact amount of coverage that medicare provides depends on how long a person. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay. How Long Will Medicaid Pay For Hospital Stay.
From audit.wa.gov.au
Management of Long Stay Patients in Public Hospitals Office of the Auditor General How Long Will Medicaid Pay For Hospital Stay Medicaid may impose limits on the length of stay for inpatient hospital services. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. The exact amount of coverage that medicare provides depends on how long a person. Payment policies differ among states and between ffs. The use of. How Long Will Medicaid Pay For Hospital Stay.
From www.youtube.com
How Long Does Medicaid Pay For Assisted Living? YouTube How Long Will Medicaid Pay For Hospital Stay In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Medicaid may impose limits on the length of stay for inpatient hospital services. Payment policies differ among states and between ffs. The use of a provider’s national provider identifier. State medicaid programs are required to cover inpatient hospital. How Long Will Medicaid Pay For Hospital Stay.
From www.ncbi.nlm.nih.gov
Figure 1, Aggregate hospital costs and hospital stays by payer, 2012 Healthcare Cost and How Long Will Medicaid Pay For Hospital Stay The use of a provider’s national provider identifier. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. These limits can vary depending on. Medicaid may impose limits on the length of stay for inpatient hospital services. State medicaid programs are required to cover inpatient hospital services, that. How Long Will Medicaid Pay For Hospital Stay.
From www.medicaidtalk.net
Does Medicaid Pay For Long Term Nursing Home Care How Long Will Medicaid Pay For Hospital Stay Base payments to hospitals pay for specific services provided to medicaid enrollees. The exact amount of coverage that medicare provides depends on how long a person. Medicaid may impose limits on the length of stay for inpatient hospital services. These limits can vary depending on. State medicaid programs are required to cover inpatient hospital services, that is, services and items. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
How Much Could Medicare Beneficiaries Pay For a Hospital Stay Related to COVID19? KFF How Long Will Medicaid Pay For Hospital Stay State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. These limits can vary depending on. Payment policies differ among states and between ffs. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Medicare covers the first 60. How Long Will Medicaid Pay For Hospital Stay.
From www.peoplekeep.com
How much does a hospital stay cost? How Long Will Medicaid Pay For Hospital Stay States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. The use of a provider’s national provider identifier. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. The exact amount of coverage that medicare provides depends on how long a person.. How Long Will Medicaid Pay For Hospital Stay.
From www.slideserve.com
PPT Understanding Medicare Barbara Childers, MSW Centers for Medicare and Medicaid Services How Long Will Medicaid Pay For Hospital Stay Payment policies differ among states and between ffs. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. The use of a provider’s national provider identifier. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration,. How Long Will Medicaid Pay For Hospital Stay.
From www.the-hospitalist.org
COVID19 Medicare data show long hospital stays, disparities The Hospitalist How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay for specific services provided to medicaid enrollees. The exact amount of coverage that medicare provides depends. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
Medicaid is the Primary Payer for LongTerm Care Services KFF How Long Will Medicaid Pay For Hospital Stay The exact amount of coverage that medicare provides depends on how long a person. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. Base payments to hospitals pay for specific services provided to medicaid enrollees. In original medicare, these are additional days that medicare will pay for when you're in. How Long Will Medicaid Pay For Hospital Stay.
From rehab-faq.com
How Long Does Medicare Pay For Rehab Inpatient And Outpatient Coverage How Long Will Medicaid Pay For Hospital Stay In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Medicaid may impose limits on the length of stay for inpatient hospital services. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. These limits can vary depending on. The use. How Long Will Medicaid Pay For Hospital Stay.
From medicarehospitalstay3dayskitsutaku.blogspot.com
Medicare Hospital Stay 3 Days How Do I Pay Medicare Premiums How Long Will Medicaid Pay For Hospital Stay States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. Medicaid may impose limits on the length of stay for inpatient hospital services. Payment policies differ among states and between ffs. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than. How Long Will Medicaid Pay For Hospital Stay.
From www.medisupps.com
How Much Does Medicare Pay for Hospital Stay Per Day? How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay for specific services provided to medicaid enrollees. These limits can vary depending on. Payment policies differ. How Long Will Medicaid Pay For Hospital Stay.
From www.medicaidtalk.net
Does Medicaid Pay For Hospital Bills How Long Will Medicaid Pay For Hospital Stay States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. Payment policies differ among states and between ffs. These limits can vary depending on. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. Medicare covers the first 60 days of a. How Long Will Medicaid Pay For Hospital Stay.
From millerestateandelderlaw.com
How Much Will Medicaid Pay Towards a Nursing Home Stay? How Long Will Medicaid Pay For Hospital Stay State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. Payment policies differ among states and between ffs. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. These. How Long Will Medicaid Pay For Hospital Stay.
From www.tffn.net
How Much Does Medicare Pay for Hospital Stay Per Day? The Enlightened Mindset How Long Will Medicaid Pay For Hospital Stay Medicaid may impose limits on the length of stay for inpatient hospital services. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. The use of a provider’s national provider identifier. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than. How Long Will Medicaid Pay For Hospital Stay.
From medicare-faqs.com
What Does Medicare Pay For Hospital Stays How Long Will Medicaid Pay For Hospital Stay Payment policies differ among states and between ffs. Medicaid may impose limits on the length of stay for inpatient hospital services. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days.. How Long Will Medicaid Pay For Hospital Stay.
From www.healthmanagement.com
Medicaid Managed Care Spending in 2019 Health Management Associates How Long Will Medicaid Pay For Hospital Stay The use of a provider’s national provider identifier. The exact amount of coverage that medicare provides depends on how long a person. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more. How Long Will Medicaid Pay For Hospital Stay.
From www.kff.org
Understanding Medicaid Hospital Payments and the Impact of Recent Policy Changes Issue Brief How Long Will Medicaid Pay For Hospital Stay In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. These limits can vary depending on. The exact amount of coverage that medicare provides depends on how long a person. The use of a provider’s national provider identifier. State medicaid programs are required to cover inpatient hospital services,. How Long Will Medicaid Pay For Hospital Stay.
From giohsonkl.blob.core.windows.net
Does Medicaid Pay For Hospital Beds at Larry Westerman blog How Long Will Medicaid Pay For Hospital Stay The exact amount of coverage that medicare provides depends on how long a person. The use of a provider’s national provider identifier. Payment policies differ among states and between ffs. Base payments to hospitals pay for specific services provided to medicaid enrollees. Medicaid may impose limits on the length of stay for inpatient hospital services. In original medicare, these are. How Long Will Medicaid Pay For Hospital Stay.
From www.medisupps.com
How Much Does Medicare Pay for Hospital Stay Per Day? How Long Will Medicaid Pay For Hospital Stay The exact amount of coverage that medicare provides depends on how long a person. The use of a provider’s national provider identifier. Base payments to hospitals pay for specific services provided to medicaid enrollees. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. State medicaid programs are required to cover inpatient hospital. How Long Will Medicaid Pay For Hospital Stay.
From www.tffn.net
How Much Does Medicare Pay for Hospital Stay Per Day? The Enlightened Mindset How Long Will Medicaid Pay For Hospital Stay The use of a provider’s national provider identifier. Payment policies differ among states and between ffs. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. State medicaid programs are required. How Long Will Medicaid Pay For Hospital Stay.
From www.medisupps.com
How Much Does Medicare Pay for Hospital Stay Per Day? How Long Will Medicaid Pay For Hospital Stay Payment policies differ among states and between ffs. Medicaid may impose limits on the length of stay for inpatient hospital services. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. The exact amount of coverage that medicare provides depends on how long a person. The use of a provider’s national. How Long Will Medicaid Pay For Hospital Stay.
From www.browardbar.org
Image for How to Get Medicaid to Pay for Some or All of Your LongTerm Care Expenses How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay for specific services provided to medicaid enrollees. The use of a provider’s national provider identifier. The. How Long Will Medicaid Pay For Hospital Stay.
From www.pinterest.com
When Will Medicaid Pay for Nursing Home Care? — StarAdvertiser Nursing home care, Medicaid How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. These limits can vary depending on. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. The exact amount of coverage that medicare provides depends on how long a person. States. How Long Will Medicaid Pay For Hospital Stay.
From www.medicaidtalk.net
Does Medicaid Pay For Hospital Bills How Long Will Medicaid Pay For Hospital Stay In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Payment policies differ among states and between ffs. State medicaid programs are required to cover inpatient hospital services, that is, services and items furnished by a hospital. Base payments to hospitals pay for specific services provided to medicaid. How Long Will Medicaid Pay For Hospital Stay.
From www.tffn.net
What Does Medicaid Pay for Home Care? Exploring Reimbursement Rates and Costs The Enlightened How Long Will Medicaid Pay For Hospital Stay The use of a provider’s national provider identifier. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. Base payments to hospitals pay for specific services provided to medicaid enrollees. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services. How Long Will Medicaid Pay For Hospital Stay.
From www.medicaidtalk.net
How Much Does Medicaid Pay For A Caregiver How Long Will Medicaid Pay For Hospital Stay In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. The use of a provider’s national provider identifier. These limits can vary depending on. Medicaid may impose limits on the length of stay for inpatient hospital services. Base payments to hospitals pay for specific services provided to medicaid. How Long Will Medicaid Pay For Hospital Stay.
From authenticmedicine.com
Medicaid Pay by Val Jones MD Authentic Medicine How Long Will Medicaid Pay For Hospital Stay Medicare covers the first 60 days of a hospital stay after a person has paid their deductible. In original medicare, these are additional days that medicare will pay for when you're in a hospital for more than 90 days. States establish and administer their own medicaid programs and determine the type, amount, duration, and scope of services within. The exact. How Long Will Medicaid Pay For Hospital Stay.