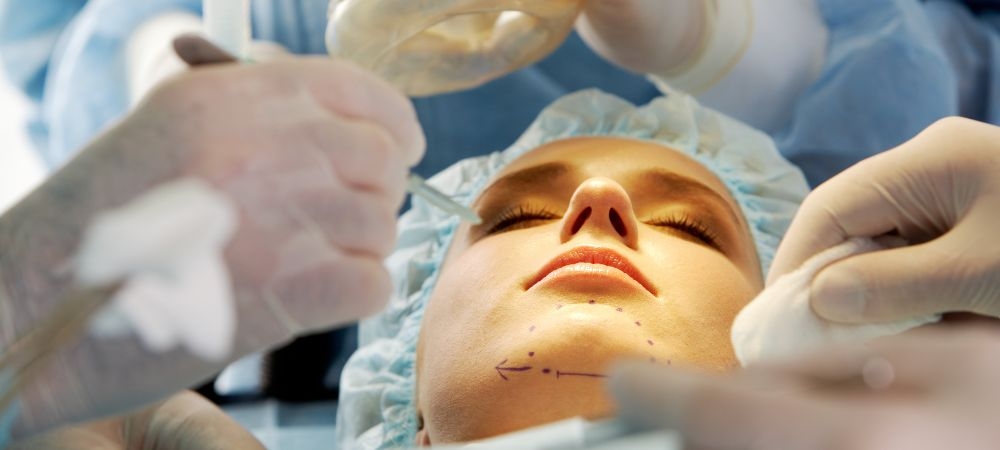

When a donor organ becomes available, it is matched to the recipient based on several criteria. This matching process involves comparing the donor's and recipient's blood types, tissue types, and other immunological factors to ensure compatibility. A close match reduces the risk of organ rejection, where the recipient's immune system may attack the new organ. In addition to compatibility, the donor organ is assessed for its condition and viability to ensure it is healthy enough for transplantation.
Intestinal Transplant: This type of transplant is less common and is performed for individuals with severe intestinal failure or disorders that significantly impair nutrient absorption and digestion. An intestinal transplant involves replacing a diseased or non-functioning intestine with a healthy one from a deceased donor. This procedure is complex and requires careful management to ensure the new intestine functions properly.
Organ transplants are a life-saving option for many individuals suffering from end-stage organ failure. However, they come with significant risks and require lifelong management. Patients must adhere to a strict regimen of medications and regular check-ups to ensure the transplanted organ remains healthy and functions properly. Despite these challenges, organ transplants offer the potential for a significantly improved quality of life and extended lifespan for individuals who might otherwise face a limited future.
Organ Allocation Systems: Organ transplant programs operate within national and regional allocation systems designed to distribute organs fairly and efficiently. These systems use complex algorithms to prioritize recipients based on medical urgency, compatibility, and time on the waiting list. While these systems aim to ensure equitable distribution, they can also contribute to variability in wait times across different regions and transplant centers.
Adherence to Medical Treatment: The ability to adhere to a strict regimen of immunosuppressive medications and regular medical appointments is a critical factor in determining eligibility. Candidates must demonstrate a history of adherence to medical treatments and the willingness to follow the complex regimen required after the transplant.
Matching Factors: The process of matching a donor organ to a recipient involves several factors, including blood type, tissue compatibility, and genetic markers. The more closely these factors align, the higher the likelihood of a successful transplant. However, finding a perfect match can be challenging and may extend the wait time. For certain organs, such as the liver, where blood type and tissue matching are crucial, the wait time can be influenced by the complexity of these matching requirements.
Living Donors: In some cases, living donors can significantly reduce wait times for certain types of transplants, particularly kidneys and livers. Living donor transplants involve a healthy individual donating a portion of their organ, which can expedite the transplant process for recipients in need. This option can help alleviate some of the wait time challenges associated with deceased donor organs.
In summary, the typical wait time for an organ transplant varies widely based on the type of organ, the recipient's medical condition, the complexity of matching factors, geographic location, and the availability of living donors. While some patients may receive a transplant relatively quickly, others may face extended wait times due to these variables. The complexity of organ transplantation underscores the importance of continued efforts to increase organ donation rates and improve allocation systems to better meet the needs of patients awaiting transplants.
Psychological and Emotional Readiness: Psychological evaluation is crucial in assessing a patient's mental and emotional readiness for the transplant process. This includes evaluating their ability to adhere to the complex regimen of post-transplant medications, follow-up care, and lifestyle changes. Mental health conditions, such as severe depression or substance abuse disorders, must be managed appropriately before proceeding with a transplant.
Overall, the eligibility criteria for an organ transplant are designed to ensure that candidates are in the best possible condition to benefit from the procedure and to maximize the chances of a successful outcome. Each transplant center may have its own specific protocols and criteria, but these general factors guide the evaluation process to determine if someone is suitable for receiving an organ transplant.
To manage these risks, healthcare providers carefully monitor the recipient's response to the medications and adjust dosages as needed. The goal is to strike a balance between effective immunosuppression and minimizing side effects. Patients are also educated on the importance of adherence to their medication regimen, as inconsistent use can increase the risk of rejection and other complications.
Long-term risks associated with organ transplants include the side effects of immunosuppressive drugs, which can lead to conditions such as high blood pressure, diabetes, and bone thinning. Additionally, recipients may face ongoing health challenges related to the transplanted organ itself, such as graft failure or complications that require further medical intervention.
Overall Health: Candidates must undergo a thorough assessment of their overall health to ensure they are physically fit to endure the transplant procedure and the subsequent recovery period. This includes evaluating their cardiovascular health, lung function, liver function, and other vital systems. Patients with significant comorbidities or uncontrolled health conditions, such as severe diabetes or infections, may be deemed ineligible until these issues are stabilized.
Exercise and Physical Activity: Engaging in regular physical activity is beneficial for overall health, improving cardiovascular fitness, and managing weight. Exercise can also help counteract some of the side effects of immunosuppressive medications, such as weight gain and reduced muscle strength. A tailored exercise program, developed in consultation with healthcare providers, can help improve physical fitness and contribute to a successful recovery.
Determining eligibility for an organ transplant involves a comprehensive evaluation process that assesses various medical, psychological, and lifestyle factors to ensure the best possible outcome for the recipient. The criteria used to determine if someone is eligible for an organ transplant include several key aspects:
Medication Adherence: One of the most crucial lifestyle changes is strict adherence to the prescribed medication regimen. Transplant recipients are required to take immunosuppressive drugs to prevent organ rejection, along with other medications to manage potential side effects and prevent infections. Consistent and accurate adherence to these medications is essential for preventing organ rejection and maintaining the health of the transplanted organ.
Liver Transplant: A liver transplant is performed when the liver has severe damage or failure, often due to conditions such as cirrhosis, liver cancer, or hepatitis. The procedure involves replacing the diseased liver with a healthy one from a donor. Liver transplants can be from living donors, who donate a portion of their liver, or from deceased donors. This type of transplant can be lifesaving and can restore normal liver function.
Immunosuppressant medications play a crucial role in organ transplant procedures by preventing the recipient's immune system from rejecting the transplanted organ. These medications are essential for the success of the transplant and are used to ensure that the new organ is accepted and continues to function properly.
Type of Organ: Different organs have varying wait times due to differences in supply and demand. For instance, wait times for kidney transplants tend to be shorter compared to those for heart or lung transplants. This is partly because kidneys are more frequently donated and have a larger donor pool compared to other organs. In contrast, organs like the heart and lungs are less commonly available, leading to longer wait times for those in need.
CureValue partners with trusted facilities and experienced doctors, ensuring that all partners meet stringent quality standards through a thorough verification process.
Users can find detailed information about sightseeing options, accessibility, transportation, living standards, and visa requirements for various destinations.
Users can contact CureValue through their website to learn more about their services and how they can help find better care elsewhere.