

Stretching exercises can be highly beneficial in rehabilitating posterior tibial tendonitis. By incorporating specific stretches that target the calf muscles, Achilles tendon, and the posterior tibial tendon itself, individuals can improve flexibility, reduce tightness, and promote healing in the affected area. Stretching helps to increase blood flow to the tendon, which can aid in the repair process and prevent further injury.
Injury-Specific Rehabilitation Often Used In Addition To Physical Therapy
Strengthening the muscles around the ankle is crucial in treating posterior tibial tendonitis. By focusing on exercises that target the muscles that support the arch of the foot and stabilize the ankle joint, individuals can improve overall foot and ankle function. Strong muscles can help alleviate stress on the posterior tibial tendon, reducing the risk of overuse and inflammation. Strengthening exercises can also improve balance and stability, which are important for preventing future injuries.
It is estimated that physicians perform 350,000 hip replacement surgeries in the US every year. There are two main types of replacements that are performed: Anterior hip replacement & Posterior hip replacements. Both of these surgeries have the same results, but the recovery process differs for each. Anterior hip replacements require a special table to […] The post You’ve Had A Hip Replacement, Now What? appeared first on Athletico.
Posted by on 2024-03-18
Have you ever wondered about the connection between knee pain, back pain, and urinary leakage? The common denominator is your hips! The hip serves as a ball and socket joint, linking the pelvis with the femur’s head (thigh bone). Its primary role is to provide dynamic stability during weight-bearing activities like walking and jogging. Approximately […] The post 3 Unexpected Reasons to Exercise Your Hips appeared first on Athletico.
Posted by on 2024-03-15
According to the U.S. Department of Health and Human Services, heart disease is the leading cause of death for both men and women in the United States. You can do many things to help decrease your likelihood of heart disease. These include: Prioritizing a healthy diet Reducing stress Maintaining a healthy weight Avoiding smoking and […] The post 3 Exercises for Better Heart Health appeared first on Athletico.
Posted by on 2024-03-13
A stroke can be a life-altering event, impacting not only the physical health but also the independence and quality of life of those affected. However, the journey to recovery is not without hope, and physical therapy plays a crucial role in helping stroke survivors regain their independence. In this blog, we will explore four key […] The post Road to Recovery: 4 Ways Physical Therapy Can Help Stroke Patients Regain Independence appeared first on Athletico.
Posted by on 2024-03-11
Using orthotic inserts or braces during rehab for posterior tibial tendonitis can provide additional support and stability to the affected foot and ankle. Orthotics can help correct any biomechanical issues that may be contributing to the condition, such as overpronation or flat feet. Braces can also help immobilize the foot and ankle, allowing the tendon to rest and heal properly. However, it is important to consult with a healthcare professional to determine the most appropriate orthotic or brace for individual needs.

Making modifications to footwear can support the healing process of posterior tibial tendonitis. Wearing supportive shoes with good arch support and cushioning can help reduce strain on the tendon and provide comfort during daily activities. Avoiding high heels and shoes with inadequate support can prevent exacerbating the condition. Additionally, custom orthotic inserts can be used in footwear to provide additional support and alignment for the foot and ankle.
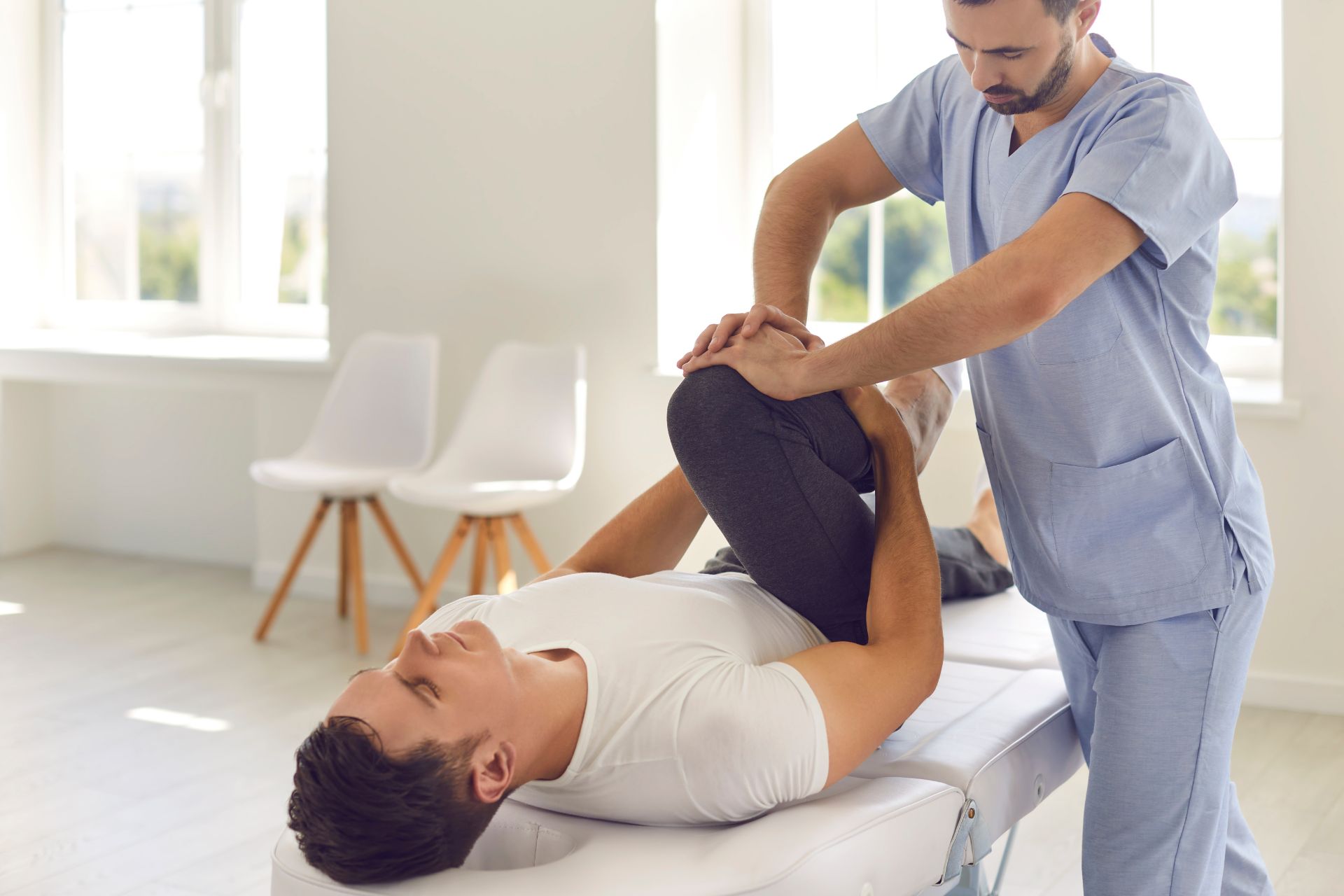
Physical therapy plays a crucial role in the rehabilitation of posterior tibial tendonitis. A physical therapist can create a customized treatment plan that includes exercises to improve strength, flexibility, and range of motion in the affected foot and ankle. They can also provide hands-on techniques such as massage and manual therapy to reduce pain and inflammation. Physical therapy can help individuals regain function and mobility in the affected area, ultimately speeding up the recovery process.
During the rehab process for posterior tibial tendonitis, it is important to avoid activities or movements that put excessive strain on the tendon. High-impact activities such as running, jumping, and sudden changes in direction should be avoided to prevent further damage. It is also recommended to avoid wearing unsupportive footwear or walking on uneven surfaces that can exacerbate the condition. Following a structured rehab program and listening to the guidance of healthcare professionals can help individuals avoid aggravating the injury.
The typical timeline for recovery from posterior tibial tendonitis with a structured rehab program can vary depending on the severity of the condition and individual factors. In general, with proper treatment and adherence to a rehab program, most individuals can expect to see improvement within a few weeks to a few months. Consistency with stretching and strengthening exercises, wearing appropriate footwear, and attending regular physical therapy sessions can help expedite the healing process and prevent future flare-ups of posterior tibial tendonitis.

Rehabilitation for hip flexor strain recovery typically involves a combination of targeted exercises, stretching routines, and manual therapy techniques aimed at improving flexibility, strength, and range of motion in the affected muscles. Physical therapists may incorporate modalities such as ultrasound, heat therapy, or electrical stimulation to help reduce pain and inflammation. Additionally, functional training exercises may be utilized to improve stability and balance in the hip region. By addressing muscle imbalances, correcting movement patterns, and gradually increasing the intensity of exercises, rehabilitation can effectively facilitate the healing process and prevent future injuries. Overall, a comprehensive rehabilitation program plays a crucial role in promoting optimal recovery and restoring function in individuals with hip flexor strains.
Rehabilitation for lumbar disc herniation typically involves a combination of physical therapy, exercises, and lifestyle modifications aimed at reducing pain, improving mobility, and preventing further injury. Physical therapy may include modalities such as heat or ice therapy, ultrasound, or electrical stimulation to help alleviate pain and inflammation. Specific exercises targeting the core muscles, such as the transverse abdominis and multifidus, can help stabilize the spine and improve posture. Additionally, stretching exercises for the hamstrings, hip flexors, and lower back muscles can help improve flexibility and reduce pressure on the affected disc. Education on proper body mechanics, ergonomics, and lifting techniques is also an important aspect of rehabilitation to prevent future episodes of disc herniation. Overall, rehabilitation aims to restore function and quality of life for individuals with lumbar disc herniation.
Ankle instability rehabilitation can benefit from a variety of strategies, including proprioceptive training, balance exercises, strength training, and neuromuscular re-education. Proprioceptive training involves activities that challenge the body's awareness of its position in space, such as balance boards or wobble cushions. Balance exercises focus on improving stability and control, often incorporating single-leg stands or dynamic movements. Strength training targets the muscles surrounding the ankle joint to improve support and stability, while neuromuscular re-education aims to improve coordination and movement patterns. Additionally, incorporating stretching and flexibility exercises can help improve range of motion and reduce the risk of injury. Overall, a comprehensive rehabilitation program that addresses all aspects of ankle instability is essential for optimal recovery and prevention of future issues.
In managing SI joint dysfunction in rehabilitation, various strategies can be implemented to address the issue effectively. These may include targeted exercises to strengthen the surrounding muscles, such as the glutes, hamstrings, and core muscles, to provide stability and support to the SI joint. Additionally, manual therapy techniques like joint mobilizations, soft tissue manipulation, and stretching can help improve joint mobility and reduce pain. Modalities such as heat therapy, ultrasound, and electrical stimulation may also be used to alleviate symptoms and promote healing. Education on proper body mechanics and posture, as well as lifestyle modifications like weight management and ergonomic adjustments, can further aid in managing SI joint dysfunction in rehabilitation. By incorporating a comprehensive approach that addresses both the physical and lifestyle factors contributing to SI joint dysfunction, rehabilitation outcomes can be optimized for the individual.